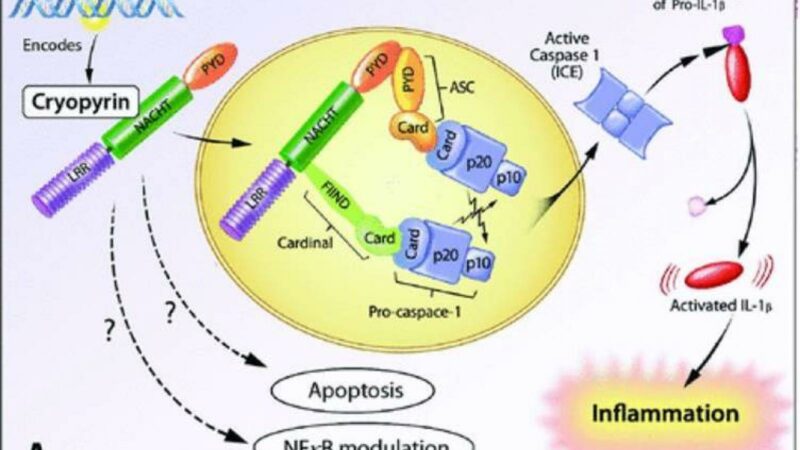
With broader awareness about the disease state, early diagnosis and treatment in autoinflammatory syndromes, and its life threatening complication Macrophage Activation Syndrome, remains a huge unmet need.
Having a “game plan” in place, and having it early, can be a life-saving experience for many patients. Abstract 1496 addresses this issue. In their study, authors implemented evidence-based guidelines into management of patients with suspected macrophage activation syndrome. As a result, they were able to shorten time to diagnosis and treatment by almost half and improved survival rate from 75% to a staggering 93.3%. Also, duration of hospital stay and use of effective treatment modalities improved significantly.
Another proof that guidelines do work.
What about the diagnostic tools? There was quite a lot presented on this topic at this year’s meeting. Abstract 1150 suggests novel markers CXCL9, CXCL10 along with IL-18 may be useful in monitoring disease course in sJIA with or without MAS. Abstract 0098 highlights CCL2 and CCR2 as chemokines involved in inflammatory responses in AOSD. All potential diagnostic tools or even treatment targets.
But what do we do while the novel markers are still being studied?
Abstract 1149 proves again usefulness of routine laboratory parameters in identifying patients at risk for MAS. As it was known before, levels of ferritin, LDH, AST and triglycerides tend to elevate in patients with sJIA and ASOD who are at the risk of MAS. Authors of the abstract propose a risk score system based on the above parameters. Their study suggests a high diagnostic value of this scoring system with specificity and sensitivity over 80%. As a matter of fact 27 out of 28 patients who developed MAS scored 5 or more in this study. Read the abstract – it’s pretty good.
All in all it seems we are getting better in diagnosing and treating autoinflammatory syndromes; an expanding auto inflammatory section in the ACR20 agenda is proof.
Related Content
-
July 21, 2016
Autoinflammatory syndromes manifest as periodic fevers in children, and are the result of…
-
January 1, 1970
Saturday's session on autoinflammatory syndromes featured Dr. Dan Kastner addressing - The Adult…
-
January 1, 1970
This podcast features a discussion of autoinflammatory and Still's disease abstracts from virtual…
-
June 11, 2020
-
May 27, 2020
This week's Tuesday Nite Rheumatology featured Dr Randy Cron from the University of Alabama…
-
May 14, 2022
Featuring Drs. Jack Cush, Olga Petryna, Bella Mehta, Rachel Tate, Yuz Yusof, discussing…